Ipamorelin 10mg
Ipamorelin is a pentapeptide that showed a significant growth hormone secretion potential both in vitro and in vivo studies. In vivo studies, it showed a similar potency and effectiveness as GHRP-6 (a synthetic growth hormone-releasing hexapeptide) as it stimulates GH release via the GHRP receptors.
What’s interesting about ipamorelin is that it did not raise ACTH (Adrenocorticotropic hormone) nor cortisol level significantly; something we’ve seen happening with GHRP-6 and GHRP-2. So, we can conclude that ipamorelin is the first GHRP-receptor agonist with GH release selectivity similar to GHRH. This is why ipamorelin is an interesting candidate for further testing.
In addition to stimulating GH secretion, this peptide has seen some interesting use in the treatment of postoperative ileus (POI), a condition characterized by transient loss of gastrointestinal motility following abdominal surgery.
The exact mechanism behind POI is a complex one, involving many different bodily structures; in addition, condition is often worsen due to the opioid drugs used for patient pain management.
In rodent studies, ipamorelin was found to selectively stimulate ghrelin (hormone produced by our stomach, affecting food intake, deposition and growth hormone release) without raising cortisol or adrenocorticotropic hormone levels. These effects were shown in both lower GI tract as well as the upper, making this peptide a viable candidate for potential POI treatment.
References:
Raun K, Hansen BS, Johansen NL, Thøgersen H, Madsen K, Ankersen M, Andersen PH. Ipamorelin, the first selective growth hormone secretagogue. Eur J Endocrinol. 1998 Nov;139(5):552-61. doi: 10.1530/eje.0.1390552. PMID: 9849822.
Greenwood-Van Meerveld B, Tyler K, Mohammadi E, Pietra C. Efficacy of ipamorelin, a ghrelin mimetic, on gastric dysmotility in a rodent model of postoperative ileus. J Exp Pharmacol. 2012 Oct 19;4:149-55. doi: 10.2147/JEP.S35396. PMID: 27186127; PMCID: PMC4863553.
$80.00
| Quantity: | 10mg |
|---|---|
| Unit: | 1 vial |
| Contents: | Ipamorelin |
| Form/Appearance: | Lyophilized/Powder |
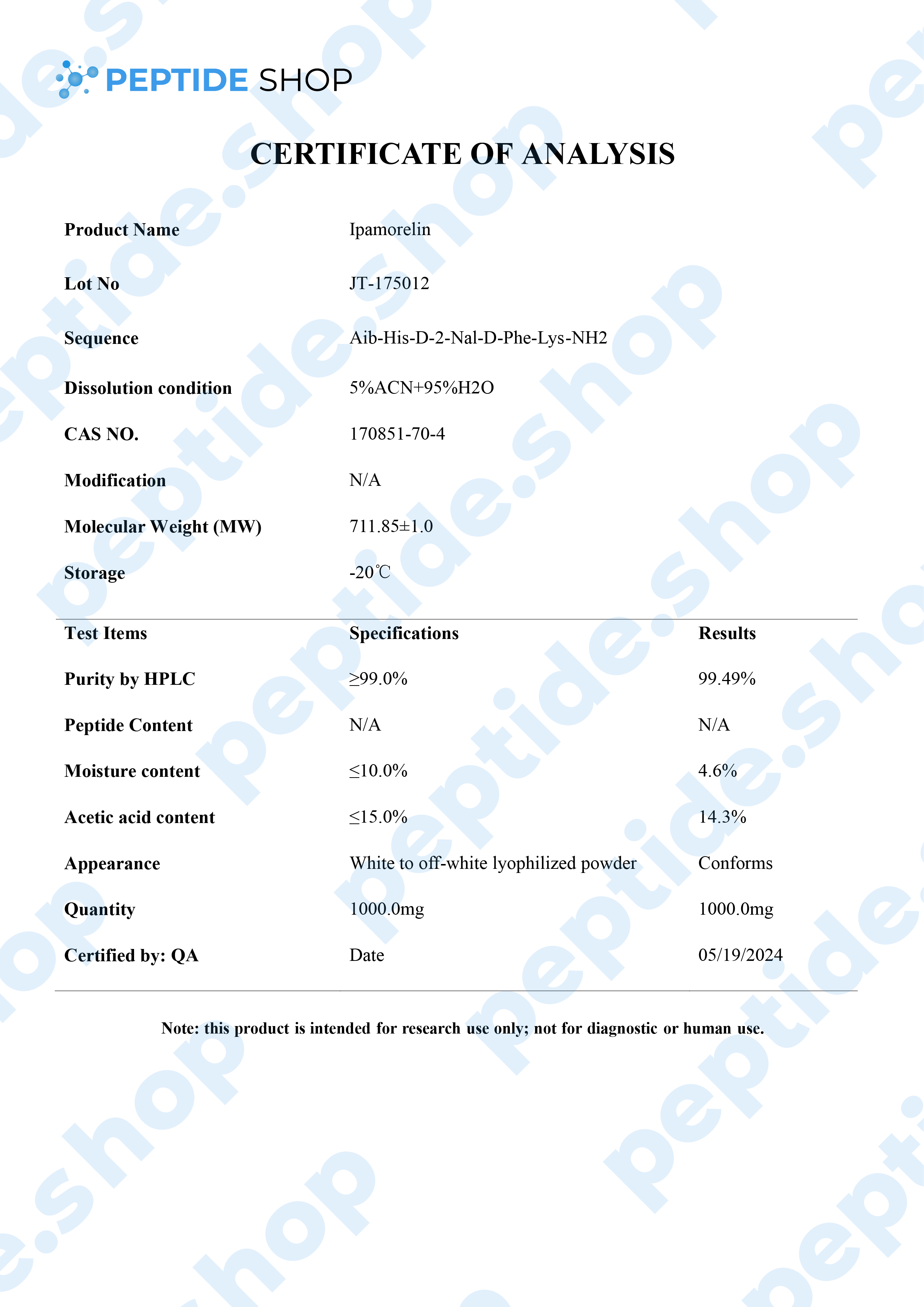
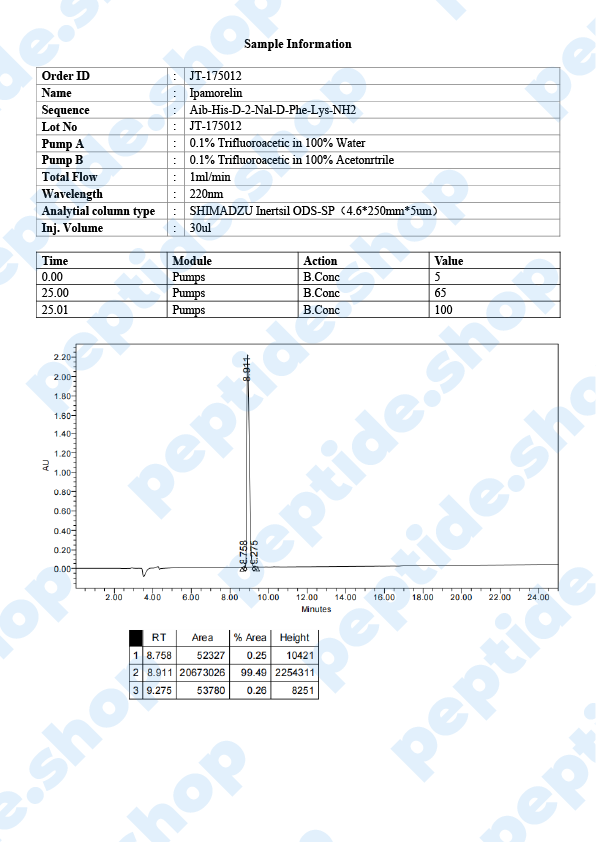
| Peptide Purity: | 99% |
| Sequence: | Aib-His-D-2Nal-D-Phe-Lys |
| Molecular Mass: | 711.87 g/mol |
| Solubility: | Sterile / Bacteriostatic water |
| Synonyms: | NNC 26-0161 |
Based on 0 reviews
|
|
|
0% |
|
|
|
0% |
|
|
|
0% |
|
|
|
0% |
|
|
|
0% |
FAQs
Related Products
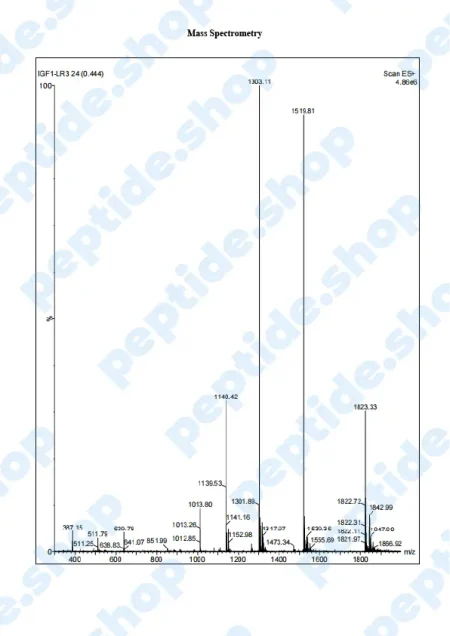
PeptideShop.com is selling insulin-like growth factor 1 (IGF-1) LR3 in vials of 3mg, in a lyophilized state, and it requires dissolution. Your choice of diluent will depend on the nature of your lab testing, but the most common ones are certainly sterile distilled water, or a sterile dilute acetic acid.
IGF-1 LR3 is based on IGF which has been chemically altered to have a prolonged half-life. This allows it to be more effective and increases the duration of its action.
IGF-1 is a 70 amino acid long peptide chain, similar in structure to insulin, which is able to bind to the insulin receptors found within the body. Insulin-like growth factor 1 is one of the principal mediators of human growth hormone (GH). What this means is IGF-1 plays a crucial role in promoting cell growth, differentiation and has a distinct anabolic effect, especially in adults.
IGF-1 LR3 And Cell Proliferation
Since IGF-1 is a part of a wide growth factor network, it plays a part in cellular proliferation and differentiation, especially in muscles and connective tissue. It also delays cell apoptosis, preventing premature cell death.
The difference between IGF-1 and IGF-1 LR3 variant is, as we said before, LR3’s longer half life; it remains in the bloodstream longer and expresses its action over a longer period.
In vitro medical studies showed that this peptide leads to the increase of muscle cells, not by hypertrophy but by actual cell division. This “side effect” proved of interest in the bodybuilding world where individuals would use (abuse) it to improve their results and get results faster. It came to a point where this peptide was declared a doping agent and banned in different high level sports competitions.
Of course, this is not something we approve of, as we are only selling peptides for laboratory testing.
IGF-1 As A Medical Disease Marker
We’re used to talking about IGF-1 and its LR3 counterpart, in the context of medical therapy and treatment, but its levels might point to a medical problem – deficiency within the body. There are many different reasons for IGF-1 deficiency, but it’s suspected that the main one is GH and growth hormone receptor defects. This is especially common in children where primary IGF deficiency is detected and treated.
IGF-1 LR3’s Effects On Myostatin Regulation
Myostatin is a protein found in muscle tissue of the skeletal system, mainly responsible for hypertrophy and cell division and differentiation. We’re not talking about muscle building here, but normal bodily muscle development during the growth period.
Deficiencies with this hormone will lead to muscle dystrophies, where affected individuals experience muscle loss, decreased quality of life as well as life expectancy. This is why researchers are so hung up on developing a IGF-1 LR3 treatment protocol that would help regulate myostatin protein, prevent muscle loss and improve the quality of life of the patients.
Sadly, we are still in the early stages of testing and research – most commonly used models are animal ones, and we have yet to see the effects of this therapy in humans.
IGF-1 LR3 Effects On Cell Aging
In addition to cell proliferation, differentiation and wound healing, some animal studies showed IGF-1 LR3 affects cellular longevity (by protecting them and prolonging apoptosis).
Besides general wellbeing, this therapy can be aimed at slowing down the progression of deteriorating diseases such as dementia or muscle dystrophy. These results have been reported in mice studies, but we should move into human testing soon.
References:
Bailes J, Soloviev M. Insulin-Like Growth Factor-1 (IGF-1) and Its Monitoring in Medical Diagnostic and in Sports. Biomolecules. 2021 Feb 4;11(2):217. doi: 10.3390/biom11020217. PMID: 33557137; PMCID: PMC7913862.
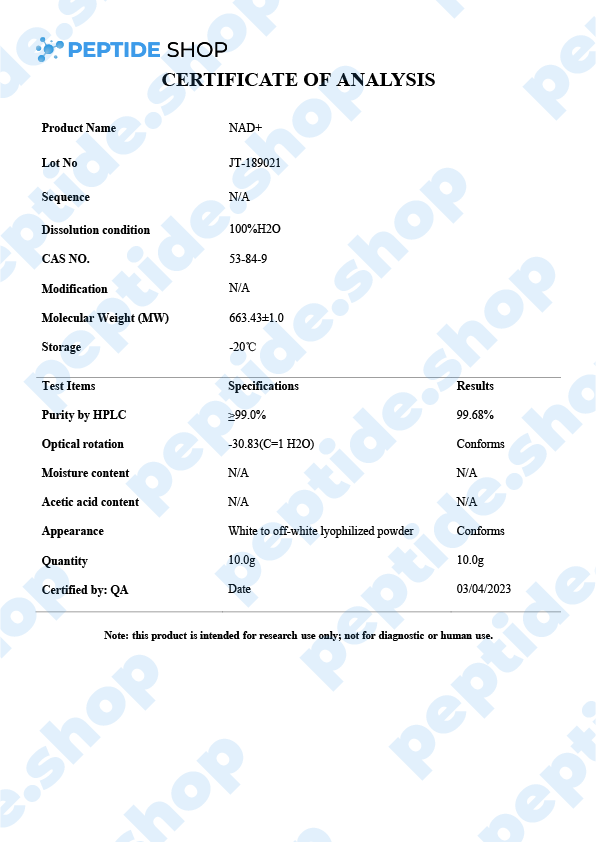
Nicotinamide adenine dinucleotide (NAD+) is a critical coenzyme that’s present in every living cell and, as such, is involved in a number of metabolic and cellular processes. This is why NAD+ is so interesting for many different areas of research such as:
- Anti aging
- Metabolic disorders
- Neurodegenerative disorders
- And even cancer research
PeptideShop.com sells NAD+ peptide in vials of 100mg and is meant for laboratory use only. Researchers commonly use it to test its effectiveness on:
- DNA damage repair and gene expression
- Stress response regulation
- Slowing down the progression of degenerative disorders
- Metabolism pathway testing
But, as previously mentioned, we are still waiting on large scale human tests.
NAD+ Role In Cellular Maintenance
Cellular NAD exists in two forms:
- NAD+
- NADH
When there’s a shift in NAD+ and its level drops in favor of NADH, this is a hallmark of aging; though the exact mechanisms that lead to this drop still remain unknown.
Naturally, numerous clinical studies showed that increasing NAD+ levels leads to the reduction of age-related immune and metabolic changes. Meaning there is potential of using NAD+ in treating age related disorders.
NAD+ And Neurodegenerative Disorders
When speaking about aging, one of the most contributing factors is mitochondrial dysfunction in neurons. Aging also speeds up the progression of neurodegenerative disorders, triggering DNA damage and mitochondrial impairment.
Luckily, studies have shown that NAD+ treatment (and even supplementation) helped restore mitochondrial function, enhance neural function and even improve cognitive abilities.
NAD+ And Metabolic Disorders
We’ve seen a dramatic increase in metabolic disorders lately, making it one of the major global health problems. Of course, we use the term metabolic disorders to cluster a whole host of problems such as obesity, diabetes, hypertension, as well as some cardiovascular pathologies.
NAD+ levels directly influence nutrient status in cells, so regulating them stands as a clear guideline to future research in hope of making NAD+ an FDA-approved way of treating metabolic and age related disorders.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7973386/
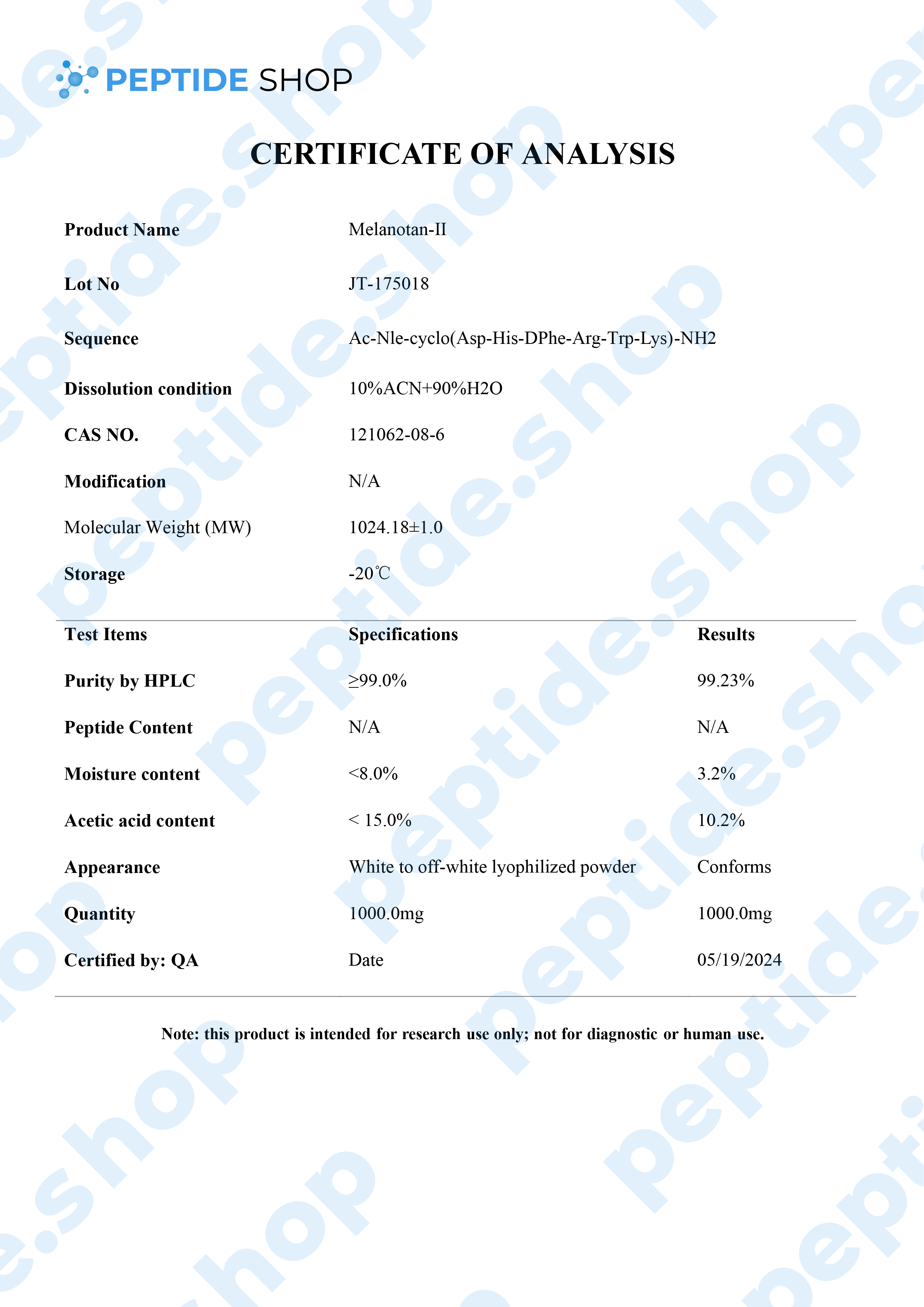
Melanotan 2 is a synthetic version of human alpha-melanocyte stimulating hormone and acts as a non selective melanocortin-receptor agonist. It was mainly developed as a sunless tanning option, but some clinical studies showed it also causes spontaneous penile erections, as well as general sexual stimulation.
Some of the other “side effects” researchers noticed were reduction in compulsive behavior, reduced glucagon production, hunger suppression and even some limited addiction control.
Melanotan 2 Effects On Autism
There is some additional recent clinical research suggesting there might be a link between Mealnotan 2 and autism. Of course, melanotan treatment cannot reverse autism, sadly, but it may act on some aspects of this disorder and make it more manageable.
In mouse model studies researchers recorded that MT2 stimulated oxytocin release, which had the potential to reduce (in some cases counteract) common ASD behaviors – behaviors that include:
- Hand clapping
- Bouncing on toes
- Body rocking
- Holding body parts in unusual positions
- Repeating vocalizations etc.
Hunger and satiety signals are controlled by serotonin, dopamine, norepinephrine and a number of other systems within our body. When talking about weight loss and appetite modulation, there are agents that do it through pure central nervous system pathways, and those that target peripheral signals (that travel to the central nervous system).
This is why we have so many different weight loss options, since medication is based on substances affecting different pathways, signals and weight management systems. One such drug, aimed at improving adipose tissue function and fatty acid metabolism is AOD9604.
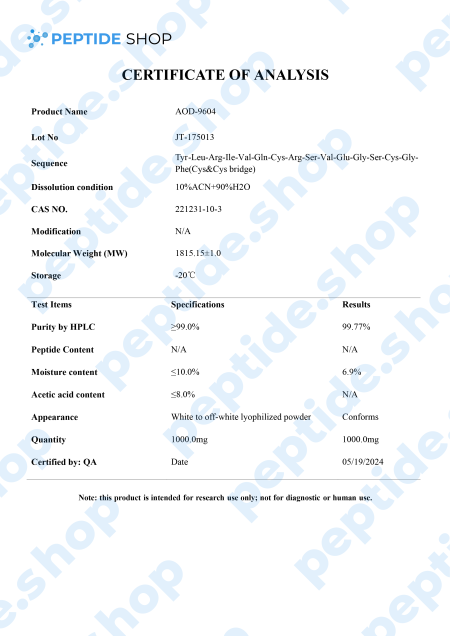
AOD9604 is a modified form of human growth hormone fragment 176-191, developed to stimulate prolipid mobilizing and lipid oxidation (during which fatty acids decompose into carbonyl compounds, unsaturated aldehydes, ketones and other substances).
Even though AOD9604 has not yet been deemed FDA-approved,a number of studies showed its administration led to a significant weight loss and improvements in glucose tolerance (in both animal and early stage human studies).
Another such study done on 300 obese individuals in Australia showed that AOD9064 administration more than tripled weight loss in test subjects, compared to those on a placebo drug. Furthermore, this study proved that long-term treatment is not likely to cause resistance to AOD9064 based medication, making it a perfect candidate for future weight loss medication and treatment.
So far, animal and human studies both showed AOD9064’s effectiveness in helping test subjects lose weight, improve glucose tolerance, while presenting with minimal side effects. Further research studies are needed before including it into an FDA-approved treatment procedure, but the initial findings show a great potential.
Reference:
Michael D. Jensen. Potential Role of New Therapies in Modifying Cardiovascular Risk in Overweight Patients with Metabolic Risk Factors. 06 September 2012
Cagrisema 10mg is one of the latest PeptideShop’s peptide blends, which combines cagrilintide and semaglutide. Each vial contains a combination of lyophilized cagrilintide and semaglutide, 5mg each, tested for purity and strength, and suitable for lab experiments and chemical trials.
Semaglutide is a GLP-1 receptor agonist. GLP-1 is one of the main gut peptide hormones in humans, which plays a role in many different mechanisms within the body from insulin secretion, glucagon release, gastric emptying, appetite and energy intake.
And cagrilintdide is an amylin analogue co-secreted with insulin, which plays a role in glycemic control and gastric emptying.
Researchers hypothesize that this combination profoundly influences receptor changes in the brain, insulin secretion, appetite regulation and glucagon secretion.
Though this combination has not yet been fully tested, we have data from a study on the effects of Cagrisema on patients with type 2 diabetes.This was a 32-week, double-blind study across 17 sites in the USA, conducted on 92 individuals in total.
Final results showed that cagrisema resulted in clinically relevant improvements in glycaemic control (significant change in HbA1c) and, more importantly, a greater weight loss versus semaglutide as well as cagrilintide.
References:
https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(23)01163-7/abstract
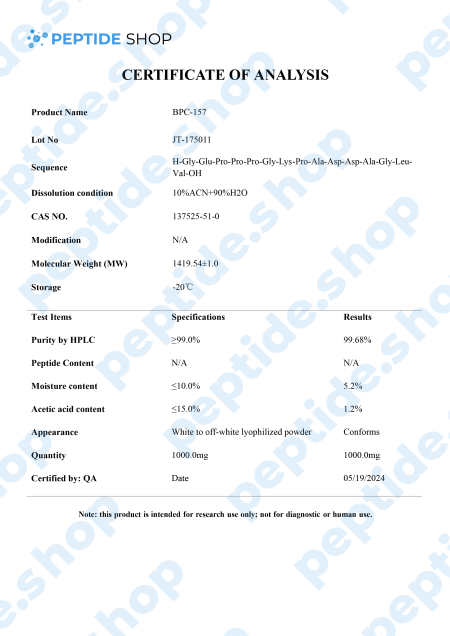
BPC-157 is a native gastric pentadecapeptide (composed of 15 amino acids), derivative of body protection compound (BPC). Being a gastric peptide allows for good oral availability and remaining stable for more than 24 hours in human gastric juice. Furthermore, there is no need for a carrier which makes this peptide unique, as compared to others that depend on it.
Clinical studies showed that BPC-157 is highly effective in both treatment and prophylaxis of various gastrointestinal lesions. This effectiveness spans to cover both acute and chronic gastric conditions, intravenous, ingastric, and even as a topical agent for deep skin burns and lesions.
Surprisingly, BPC-157 has also shown a beneficial effect on:
- Brain lesions – in one of the most recent studies researchers concluded that BPC-157 expressed a direct therapeutic effect in rat test subjects following a stroke. This peptide not only delayed neural damage, but also promoted full functional recovery.
- Behavioral disorders – medical research showed that BPC-157 counteracted catalepsy (a state of a trance or a seizure) in rat models. This research indicated a connection between BPC-157 and dopamine as well as glutamate and nitric oxide system (vital in schizophrenia therapy).
- Spinal cord injuries – A particularly interesting study showed that BPC-157 administration to rats with spinal cord injuries resulted in improvements mere 10 minutes after the initial dosage. On the contrary, untreated rats did not fully recover days, weeks, months and, in some rare cases, years following the injury.
In conclusion, we saw BPC-157 application results in a myriad of beneficial effects in various different systems within the body. Of course, many of these studies were performed on animal test subjects and we’re going to need additional ones to clarify its effect in humans and the full extent of its therapeutic potential.
References:
Vukojevic J, Milavić M, Perović D, Ilić S, Čilić AZ, Đuran N, Štrbe S, Zoričić Z, Filipčić I, Brečić P, Seiverth S, Sikirić P. Pentadecapeptide BPC 157 and the central nervous system. Neural Regen Res. 2022 Mar;17(3):482-487. doi: 10.4103/1673-5374.320969. PMID: 34380875; PMCID: PMC8504390.
Sikiric P, Hahm KB, Blagaic AB, Tvrdeic A, Pavlov KH, Petrovic A, Kokot A, Gojkovic S, Krezic I, Drmic D, Rucman R, Seiwerth S. Stable Gastric Pentadecapeptide BPC 157, Robert’s Stomach Cytoprotection/Adaptive Cytoprotection/Organoprotection, and Selye’s Stress Coping Response: Progress, Achievements, and the Future. Gut Liver. 2020 Mar 15;14(2):153-167. doi: 10.5009/gnl18490. PMID: 31158953; PMCID: PMC7096228.
Tesamorelin is a 44 amino acid long, synthetic growth hormone releasing hormone (GHRH) analogue. It was primarily developed and used to treat visceral fat buildup in HIV positive patients suffering from lipodystrophy (a condition characterized by abnormal fat distribution).
Tesamorelin peptide activates GHRH receptors in the pituitary gland, resulting in growth hormone synthesis and release. This GH release further stimulates the production of Ilike growth factor-1 (IGF-1), which is naturally low in obese and diabetic patients.
The good thing about tesamorelin is that it was approved in the US back in 2010 for the treatment of abdominal fat in HIV positive patients as a part of the antiviral therapy-related lipodystrophy. It has also been evaluated as a potential therapy of insulin resistance, nonalcoholic fatty liver and, of course, obesity. These clinical studies are still ongoing and we’ll need more information to confirm its effectiveness.
The usual tesamorelin dosage for patients is 2mg given in the form of a subcutaneous injection, once a week. As for the side effects, patients did not report that many, but from the ones we have documented, most common are:
- Application site irritation
- Itching
- Peripheral edema
- Mild nausea
- Redness
More importantly, tirzepatide therapy was not associated with hepatotoxicity and is very unlikely to cause any clinically apparent liver injuries.
Reference:
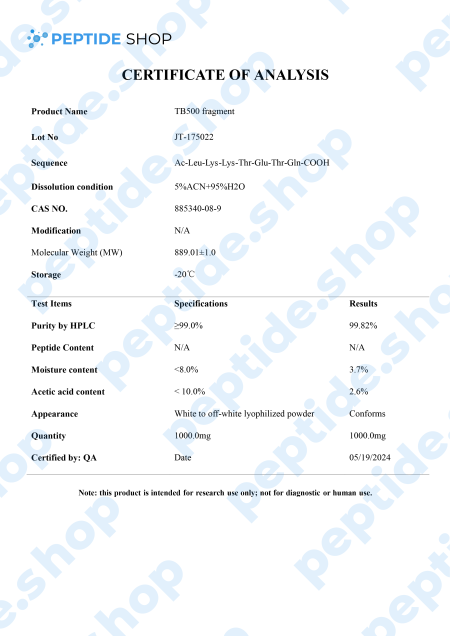
TB-500 is a 43 amino acid long synthetic peptide, analogue of thymosin beta-4. Thymosin beta-4 is a widely distributed peptide, and present in virtually all mammalian cells, which plays a pivotal role in many different processes in the body – it increases angiogenesis (formation of new blood vessels), proliferation, inhibits apoptosis (cell death) and inflammation.
Numerous animal clinical trials also showed that thymosin beta-4 can be used to indicate myocardial, liver and renal problems.
Angiogenesis:
Thymosin beta-4 promotes angiogenesis, triggers cell proliferation and migration, as well as the formation of capillary-like structures in cells. It also triggers blood perfusion (local fluid flow) by increasing capillary density.
Apoptosis:
Thymosin beta-4 inhibits apoptosis by inhibiting the transforming growth factor pathway. It also prevents nucleus pulposus (spinal disk providing shock absorption during movement) cell apoptosis and slows down cellular aging.
Inflammation:
In mouse models Tβ4 significantly dropped the number of inflammatory cells in the brains of the treated animals. It also prevented the production of proinflammatory cytokines and effectively blocked the increase of ethanol-induced inflammatory factors.
Heart Health:
Clinical data showed that thymosin beta-4 has a positive effect on both acute phase (immediately following the injury) where it preserves the ischemic myocardium, as well as in the chronic phase, in which it activates the growth of vascular cells.
After observing Tβ4’s benefits in animal models, it’s not surprising TB-500 gained so much popularity recently, since it acts as Tβ4’s synthetic analogue. Numerous clinical studies (in animal models) showed TB-500 as a potent way to improve blood vessel growth and fluid flow, accelerate wound healing, reduce oxidative stress and bind protein.
Of course, more research is needed to determine the full effects of this peptide, its safety and effectiveness in human test subjects.
Reference:
Xing Y, Ye Y, Zuo H, Li Y. Progress on the Function and Application of Thymosin β4. Front Endocrinol (Lausanne). 2021 Dec 21;12:767785. doi: 10.3389/fendo.2021.767785. PMID: 34992578; PMCID: PMC8724243.
Growth hormone replacement therapy has long been accepted as one of the most effective ways of treating GH deficiency and related conditions. This therapy uses recombinant human growth hormone (rhGH) and, despite its longstanding usage record, it has been surrounded by controversy. Even though, in the short term, this therapy is very effective, when it comes to long term effects, issues start to arise:
- Long term improper dosage can lead to some severe side effects
- This therapy may affect normal physiology after prolonged application
- Some federal regulations might interfere with the therapy
- There’s even some concerns that this therapy may awaken latent cancers and cause metabolic disorders
There is one more major problem with dosage because the body can’t properly modulate tissue exposure to rhGH. Meaning, the practitioner uses their “best guess” to access the appropriate dosage.
This is why researchers are looking for alternative ways to stimulate GH production by targeting GH secretagogues and promoting pituitary gland health. One such molecule is sermorelin, a GHRH analog that impacts the hypothalamic-pituitary-pituitary-somatotropic axis.
It’s used for both treatment and diagnosis of GH deficiency as research studies showed sermorelin promoted change in GH levels similar to those observed with endogenous GHRH. It also stimulates FSH (follicle-stimulating hormone) and LH (luteinizing hormone), which implies a potential role in the treatment of hypogonadism.
Though we need larger, longitudinal studies, sermorelin proved as a promising GH and IGF-1 stimulator and diagnostic agent.
Reference:
Walker RF. Sermorelin: a better approach to management of adult-onset growth hormone insufficiency? Clin Interv Aging. 2006;1(4):307-8. doi: 10.2147/ciia.2006.1.4.307. PMID: 18046908; PMCID: PMC2699646.
Sinha DK, Balasubramanian A, Tatem AJ, Rivera-Mirabal J, Yu J, Kovac J, Pastuszak AW, Lipshultz LI. Beyond the androgen receptor: the role of growth hormone secretagogues in the modern management of body composition in hypogonadal males. Transl Androl Urol. 2020 Mar;9(Suppl 2):S149-S159. doi: 10.21037/tau.2019.11.30. PMID: 32257855; PMCID: PMC7108996.
Oxytocin, also known as the love hormone, helps us bond with our loved ones and is often released through touch, exercise, and music.
What is Oxytocin?
This natural hormone manages crucial aspects of male and female reproductive systems, including lactation, labor, delivery, and certain aspects of human behavior. The hypothalamus produces oxytocin, but the posterior pituitary gland releases and stores this hormone into the bloodstream.
Hormones are chemicals that manage various functions in the human body by carrying messages through blood to tissues, muscles, and organs. These signals instruct your body what to do and when to do it.
The hypothalamus is part of the brain that controls functions such as heart rate, digestion, body temperature, and blood pressure. On the other hand, the pituitary gland is a small, pea-sized endocrine gland placed at the base of the brain, below the hypothalamus.
Synthetic Forms of Oxytocin
A synthetic form of oxytocin is used in hospital settings, particularly when doctors need to induce labor in childbirth if it hasn’t begun naturally or to help with contractions. Healthcare providers may also use this hormone to speed up the delivery of the placenta, which is the third stage of labor, and minimize the risk of heavy bleeding.
Function of Oxytocin
As previously mentioned, the two main functions of oxytocin are to encourage uterine contractions in childbirth and labor and to boost contractions of breast tissue to help with lactation after childbirth.
However, apart from these, oxytocin has other important roles, such as:
- Placenta-infant bonding
- Romantic attachment
- Trust
- Recognition
- Sexual arousal
The effects of oxytocin on the human brain are complex, and scientists are currently researching the role of oxytocin in various conditions.
- PTSD
- Depression
- Autism spectrum disorder
- Anxiety
- Anorexia
- Addiction
Florea T, Palimariciuc M, Cristofor AC, Dobrin I, Chiriță R, Bîrsan M, Dobrin RP, Pădurariu M. Oxytocin: Narrative Expert Review of Current Perspectives on the Relationship with Other Neurotransmitters and the Impact on the Main Psychiatric Disorders. Medicina (Kaunas). 2022 Jul 11;58(7):923. doi: 10.3390/medicina58070923. PMID: 35888641; PMCID: PMC9318841.
Kendrick KM, Guastella AJ, Becker B. Overview of Human Oxytocin Research. Curr Top Behav Neurosci. 2018;35:321-348. doi: 10.1007/7854_2017_19. PMID: 28864976.
https://www.sciencedirect.com/science/article/pii/S0306453013002369
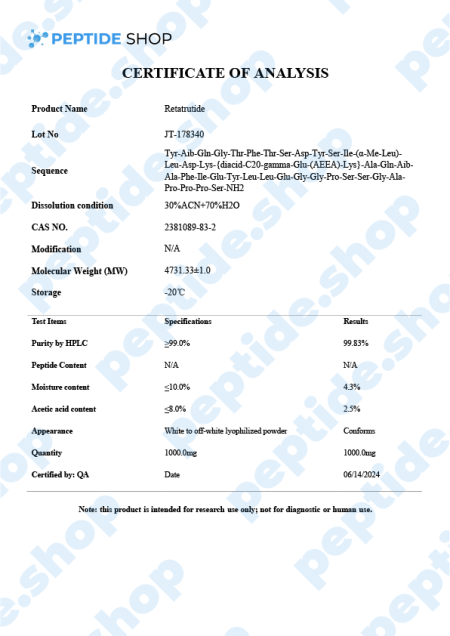
Retatrutide is one of the latest incretin mimetic drugs being tested for their weight reduction properties. Researchers use incretin mimetic agents as they work to mimic incretin hormones (gut peptides that get secreted after we eat) to allow for a better insulin secretion and hyperglycaemic control.
Even though there are numerous weight reduction agents being prescribed and used, FDA-recognized “treatment” for nonsyndromic obesity are:
- Orlistat
- Phentermine-topiramate
- Naltrexone‐bupropion
- Liraglutide and
- Semaglutide
With the exception of glucagon-like peptide 1 receptor agonists (such as semaglutide), most weight reduction agents come with a specific set of side effects such as nausea, gastrointestinal distress, abdominal pain, vomiting, diarrhea, or a general weight decrease that does not cross the 15% mark. Some of these medications even come with a warning against using them if a patient is suffering from a kidney, heart, thyroid or any related problems.
This is why scientists are turning more and more to retatrutide, because this incretin mimetic decreases appetite, promotes the feeling of fullness and slows down the process of gastric emptying, but does all that while presenting with minimal side effects and increased weight loss effectiveness, compared to liraglutide or semaglutide.
Retatrutide Mechanism of Action
Retatrutide exerts a powerful glucagon-receptor agonistic effect. When we compare it to human glucagon and glucagon-like peptide 1 (GLP-1), it exhibits:
- Reduced potency on the GCGR (human glucagon receptor) and GLP-1R (glucagon-like peptide-1 receptor)
- Enhanced potency at the human GIPR (gastric inhibitory polypeptide receptor)
When talking about in vitro experiments, retatrutide demonstrated similar efficacy in evoking glucose production within hepatocytes and inducing lipolysis. Also, retatrutide showed a favorable half-life of 6 days, enabling it a weekly dosage regimen (should the drug get FDA approved).
Another double-blind study conducted in the US on obese patients showed promising results. 338 adults in total were involved, split into 6 cohorts (depending on the weekly dosage), up against a placebo group. Retatritude group experienced the following results:
- 1mg group – after 24 weeks this group experienced weight loss of 7.2%, and after 48 weeks a total loss of 8.7%
- 4mg group (commencing with 2mg) – after 24 weeks this group experienced a weight loss of 11.8%, and after 48 weeks a total loss of 16.3%
- 4mg group (commencing with 4mg) – after 24 weeks this group experienced a weight loss of 13.9%, and after 48 weeks a total loss of 17.8%
- 8mg group (commencing with 2mg) – after 24 weeks this group experienced a weight loss of 16.7%, and after 48 weeks a total loss of 21.7%
- 8mg group (commencing with 4mg) – after 24 weeks this group experienced a weight loss of 17.9%, and after 48 weeks a total loss of 23.9%
- 12mg group (commencing with 2mg) – after 24 weeks this group experienced a weight loss of 17.5%, and after 48 weeks a total loss of 24.2%
In contrast, the placebo group only experienced a 1.6% weight loss after 24 weeks and 2.1% after 48. Findings also showed that adverse effects related to retratitude treatment (such as nausea, vomiting, diarrhea and constipation), were mild and depended on the dosage.
In conclusion, this peptide showed promising results in addressing obesity in both in vitro and human test subject studies. However, test samples were relatively small, and we still need more research and clinical trials to show the effectiveness of retratutide as an effective, long-term way of managing weight.
Reference:
Naeem M, Imran L, Banatwala UESS. Unleashing the power of retatrutide: A possible triumph over obesity and overweight: A correspondence. Health Sci Rep. 2024 Feb 5;7(2):e1864. doi: 10.1002/hsr2.1864. PMID: 38323122; PMCID: PMC10844714.
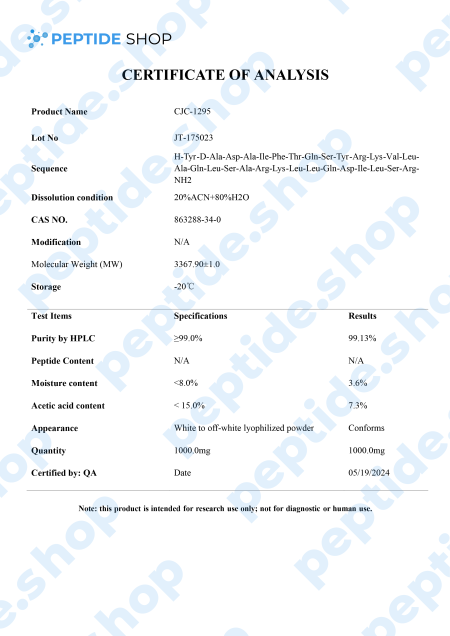
If you’re a peptide researcher (or plan on becoming one), you should know the difference between CJC-1295 and CJC-1295 DAC. CJC-1295 DAC features an additional component at the end of the peptide chain, also known as a drug affinity complex or DAC.
This small fragment changes the peptide’s functionality and extends its half-life to six to eight days. It might have a prolonged effect of up to two weeks.
Below, we will showcase the main similarities and differences between these two peptides, including their properties, characteristics, and mechanism of action.
What is CJC-1295 DAC peptide?
This peptide resembles the regular CJC-1925 since it is a modified form of natural GHGR (1-29). However, this one differs from CJC-1925. It has an additional molecule known as a “drug affinity complex.”
DAC features a couple of oxygen and nitrogen atoms connected by chemical bonds. According to some findings, this small number of atoms could significantly impact peptide breakdown rate and its use in the body.
What is CJC-1295 Peptide?
This peptide is also known as “modified growth hormone releasing factor (1-29)”, “ModGRF 1-29”, or “Modified GRF (1-29).” You may also encounter the name “CJC-1295, without DAC.”
All these names imply a specific peptide molecule containing a short amino acid chain. As many studies have indicated, this peptide may boost growth hormones in the bloodstream.
Growth hormone may have a significant role in several vital internal activities. It could facilitate cellular reproduction, repair, and growth, help with tissue repair, improve muscle cell development, support skin cells, and other functions.
While the body naturally produces growth hormone, this production tends to naturally decrease. According to some research done in laboratory settings, CJC-1295 may encourage the natural production of growth hormone, increasing its levels, which could lead to quicker repair, fat cell burn, and muscle cell growth.
Differences between CJC-1295 DAC and CJC-1295
As research studies have outlined, here are some fundamental differences between these two peptides.
Half-life
The main distinction lies in their half-lives. CJC-1295 is thought to mimic the body’s natural peptide. The endogenous GHRH has a short half-life of just a couple of minutes. Similarly, CJC-1295 has a brief half-life of around half an hour.
Regarding the second peptide, the additional DAC could significantly alter the organism’s peptide use. Researchers believe that DAC offers a peptide, a lysine linker, which could protect and prevent it from degrading.
Moreover, the DAC component could extend the half-life of this peptide to about six to eight days.
Properties of CJC-1295 DAC peptide
It is believed that CJC-1295 DAC boosts growth hormone levels in the bloodstream. Additionally, several studies suggest the following:
- Scientists and researchers need to focus their attention to studying the potential of growth hormones on growth and muscle recovery.
- Growth hormone may help convert fatty tissue into energy.
- Growth hormones are linked with collagen production in the skin, which means this peptide may also help with skin regeneration and skin cell development.
- CJC-1295 DAC may positively impact sleep patterns.
- Growth hormone is essential for tissue regeneration and helps the organism recover from damage.
References:
Teichman SL, Neale A, Lawrence B, Gagnon C, Castaigne JP, Frohman LA. Prolonged stimulation of growth hormone (GH) and insulin-like growth factor I secretion by CJC-1295, a long-acting analog of GH-releasing hormone, in healthy adults. J Clin Endocrinol Metab. 2006 Mar;91(3):799-805. doi: 10.1210/jc.2005-1536. Epub 2005 Dec 13. PMID: 16352683.
Sam L. Teichman, Ann Neale, Betty Lawrence, Catherine Gagnon, Jean-Paul Castaigne, Lawrence A. Frohman, Prolonged Stimulation of Growth Hormone (GH) and Insulin-Like Growth Factor I Secretion by CJC-1295, a Long-Acting Analog of GH-Releasing Hormone, in Healthy Adults, The Journal of Clinical Endocrinology & Metabolism, Volume 91, Issue 3, 1 March 2006, Pages 799–805,
American Journal of Physiology-Endocrinology and Metabolism 2006 291:6, E1290-E1294


 Anti Aging
Anti Aging Hair Growth
Hair Growth Muscle Growth
Muscle Growth Peptide Blends
Peptide Blends Peptide Supplies
Peptide Supplies Peptides
Peptides Skin
Skin Testosterone
Testosterone Weight Loss
Weight Loss










Reviews
There are no reviews yet.